How legionella fits RIDDOR reporting explained
- 3h
- 9 min read

If you manage compliance for a healthcare or commercial facility, you have almost certainly encountered the question: does a positive legionella test mean you must file a RIDDOR report? The short answer is no, and misunderstanding how legionella fits RIDDOR reporting causes two costly problems: facilities either over-report routine monitoring results or, far more dangerously, miss genuine reporting obligations when an employee actually contracts legionellosis. This article cuts through the confusion, explains precisely what triggers a RIDDOR obligation, and shows how your day-to-day control measures directly support your ability to report correctly and confidently.
Table of Contents
Key Takeaways
Point | Details |
Separate duties clarified | Legionella control focuses on prevention; RIDDOR reporting applies only when an employee contracts legionellosis linked to work exposure. |
RIDDOR reporting triggers | Report confirmed legionellosis in employees exposed to likely contaminated cooling towers or water systems. |
Critical control measures | Maintain water temperatures (hot above 60°C/50°C, cold below 20°C), regular flushing, and cleaning to reduce legionella risk. |
Record keeping essentials | Detailed, dated temperature and maintenance logs support effective compliance and evidence for RIDDOR reports. |
Distinct public health notifications | Clinical legionellosis reporting to UKHSA is separate from employer RIDDOR duties and has different timelines. |
Understanding legionella control versus RIDDOR reporting
These are two separate legal duties, and conflating them is where most compliance errors begin. Legionella risk management sits primarily under the Control of Substances Hazardous to Health (COSHH) Regulations and ACOP L8. It covers your ongoing obligations: legionella monitoring duties such as temperature checks, flushing regimes, risk assessments, and written control schemes. These apply continuously, regardless of whether anyone falls ill.
RIDDOR, the Reporting of Injuries, Diseases and Dangerous Occurrences Regulations 2013, operates on a completely different trigger. As HSE makes clear, RIDDOR reporting is about a workplace-linked case of disease, not routine legionella test results alone. That distinction is fundamental. A positive water sample from your cooling tower is a control failure requiring immediate remediation. It is not, by itself, a RIDDOR event.
There is also a third pathway many facilities managers overlook entirely. Legionellosis notification to public health is principally carried out by clinicians reporting to the UK Health Security Agency (UKHSA) within 3 days. That is the doctor’s responsibility, not yours. Your RIDDOR obligation and the clinician’s public health notification are distinct, parallel duties that can both arise from the same case.
To summarise the three duty areas clearly:
Legionella risk management: Continuous, duty-holder led, governed by COSHH and ACOP L8
RIDDOR reporting: Employer-triggered, only on confirmed workplace-linked legionellosis in an exposed employee, reported to HSE
Public health notification: Clinician-led, reported to UKHSA within 3 days of confirmed or probable diagnosis
With a clear understanding of these distinct duties, you can now explore precisely when RIDDOR reporting is triggered by a legionella case.
When legionella cases must be reported under RIDDOR
The trigger is specific. You must report cases of legionellosis in an employee who has worked on cooling towers or hot and cold water systems likely to be contaminated. Three elements must align before a RIDDOR obligation arises:
A diagnosed case of legionellosis: The employee must have a confirmed or probable clinical diagnosis, not simply elevated antibody titres or an inconclusive screen.
Workplace exposure: The employee must have been working with or around systems capable of generating and dispersing legionella-containing aerosols, such as cooling towers, spa pools, or hot and cold water networks.
Likely contamination: The system conditions at the time of exposure must have been such that legionella growth was plausible. This means temperatures in the growth range, stagnation, biofilm, or documented control failures during the exposure window.
That third element, “likely to be contaminated,” is where your routine monitoring records become legally critical. If your temperature monitoring checks show consistently compliant readings in the period before illness, that is material evidence. If records show missed checks, exceedances, or gaps, it strengthens the case that the system was likely contaminated during the relevant period.
The moment you suspect a RIDDOR legionella case, act immediately on four fronts:
Obtain the clinical diagnosis details and confirm the legionellosis strain where possible.
Identify which systems the employee had access to and the nature of any aerosol-generating exposure.
Retrieve all control records covering the exposure window, including temperature logs, flushing records, and any maintenance or remediation entries.
Assess whether those records indicate the system was “likely to be contaminated” at the time.
Pro Tip: Do not wait for formal confirmation of the RIDDOR legionella case before pulling your records. Retrieval delays can compromise the accuracy of your exposure narrative and leave you unable to demonstrate adequate control.
Once you have confirmed all three trigger elements, report via the HSE online reporting portal as a reportable disease under RIDDOR. Knowing when to report, facilities managers must ensure proper environmental controls both to prevent illness and to support defensible RIDDOR compliance.
Legionella control measures supporting RIDDOR compliance
Your control programme and your RIDDOR readiness are not separate workstreams. They are the same thing viewed from different angles. HSE requires hot water stored above 60°C, distributed above 50°C, and cold water below 20°C, with regular flushing and cleaning throughout the system. These thresholds exist because legionella bacteria multiply most aggressively between 20°C and 45°C.
Control measure | Target | Frequency |
Hot water storage temperature | ≥ 60°C | Monthly sentinel outlet checks |
Hot water distribution temperature | ≥ 50°C at outlets | Monthly sentinel outlet checks |
Cold water storage temperature | < 20°C | Six-monthly tank inspection |
Infrequently used outlet flushing | Full flush to drain | Weekly |
Showerhead and hose cleaning | Dismantle, descale, disinfect | Quarterly |
Cold water tank inspection | Visual check, condition report | Six-monthly |
Maintaining these controls consistently does two things simultaneously. It reduces the probability of legionella growth reaching infectious concentrations, and it generates the dated evidence base you need to assess “likely contamination” if a RIDDOR legionella case ever arises.

Routine temperature monitoring records help demonstrate that systems were controlled during the relevant period for any employee legionellosis case. In practice, this means your logbook entries are as much a legal document as they are an operational tool. Gaps, undated entries, or inconsistent readings are not just compliance failures. They are liability gaps.
Key areas your control records must cover:
Sentinel outlet temperatures recorded with date, time, outlet location, and operative name
Flushing records including outlet ID, flush duration, and any observations
Remediation actions taken following any exceedances, with close-out dates
Cleaning and disinfection certificates for tanks, cooling towers, and showerhead servicing
Pro Tip: An automated temperature monitoring system removes the single biggest weakness in most manual programmes: human inconsistency. Continuous electronic records with timestamps are far more defensible in a RIDDOR investigation than handwritten logbooks with occasional gaps.
With control measures clearly defined, it is worth comparing RIDDOR duties to other legionella-related reporting pathways to clarify where each responsibility sits.
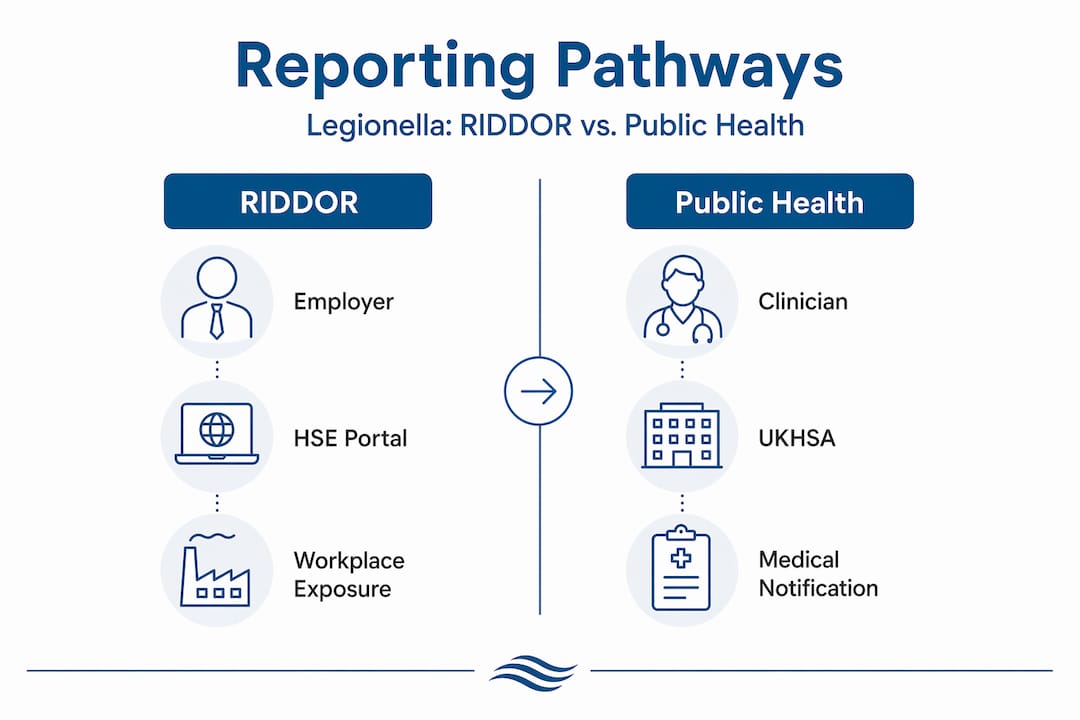
Comparing RIDDOR and public health legionella reporting
These two pathways are frequently confused, and that confusion carries real risk. If you believe the doctor’s notification to UKHSA covers your RIDDOR obligation, you may miss a statutory deadline and face enforcement action.
Feature | RIDDOR reporting | UKHSA public health notification |
Who reports | Employer (dutyholder) | Registered medical practitioner (clinician) |
Reported to | HSE | UKHSA |
Legal basis | RIDDOR 2013 | Health Protection (Notification) Regulations 2010 |
Trigger | Workplace-linked legionellosis in exposed employee | Confirmed or probable legionellosis diagnosis |
Deadline | Without delay (as soon as practicable) | Within 3 days of diagnosis |
Your responsibility | Yes | No (clinician’s duty) |
Clinicians report legionellosis to UKHSA under separate Health Protection Notification rules within 3 days. You have no control over that process, and you cannot rely on it as a substitute for your own RIDDOR submission.
The practical takeaway is straightforward. If an employee is diagnosed with legionellosis and you can establish a plausible exposure link to your water systems, do not wait to see whether a public health notification triggers some other process. Assess the RIDDOR criteria independently and report if they are met. The legionella control approaches relevant to your sector will determine the specific system types you need to consider in that exposure assessment.
Having clarified reporting pathways, the focus now shifts to practical steps for aligning your legionella control programme with RIDDOR readiness.
Practical steps for legionella management and RIDDOR readiness
Genuine RIDDOR readiness is not a separate project. It is the natural outcome of a well-maintained legionella control programme. The following steps bring both together.
Conduct and regularly review a full legionella risk assessment covering all water systems, citing COSHH and ACOP L8 guidance. Review it at least every two years or following significant changes to the building, occupancy, or water systems. You can find a detailed breakdown of what that involves in our legionella risk assessment guidance.
Implement a written control scheme specifying responsible persons, frequencies, temperature targets, flushing schedules, and escalation actions for exceedances.
Identify sentinel outlets for monthly temperature checks and ensure they represent the range of system conditions across your premises.
Maintain detailed, dated records of all monitoring activities, including who carried out the check, the result, and any action taken. Undated records are functionally worthless in a RIDDOR investigation.
Prepare exposure narratives in advance by maintaining a clear map of which employees have routine contact with which water systems. If a case arises, you can move quickly to establish or rule out workplace exposure.
Aligning monitoring schedules to HSE temperature expectations and maintaining detailed logs for timely retrieval is the foundation of defensible RIDDOR reporting for legionellosis. Every action recorded in your logbook is a piece of evidence you may need to call upon.
Additional operational measures that directly support RIDDOR readiness:
Keep an up-to-date register of all water system assets, including age, condition, and last service date
Document any periods of low or no occupancy where stagnation risk increases, particularly relevant post-pandemic or in seasonal buildings
Run annual temperature monitoring procedures refresher training for responsible persons so records remain consistent in quality and format
Conduct a legionella risk assessment review immediately following any significant change to water system configuration
Pro Tip: Treat your logbook as the document you would hand to an HSE inspector the morning after a reported legionellosis case. If that thought makes you uncomfortable, your records need attention now, not after an incident.
Rethinking legionella RIDDOR reporting: lessons from practice
Here is something most guidance documents do not say plainly: the biggest RIDDOR compliance failures we see are not from deliberate evasion. They come from genuine confusion about what the duty actually requires.
Facilities managers who believe any positive legionella water sample triggers a RIDDOR submission end up in one of two bad places. They either over-report, which draws unnecessary regulatory scrutiny, or they become so conditioned to treating positives as “just a control issue” that they fail to assess whether an employee has actually fallen ill with a workplace-linked illness. RIDDOR submissions focus on establishing an exposure link supported by temperature logs, not on lab results alone.
The second common failure is documentary. When a legionellosis case does arise and investigators ask for records covering the six weeks before symptom onset, too many facilities teams find inconsistent logbooks, missed monitoring dates, or entries made retrospectively. At that point, even if your systems were genuinely well-controlled, you cannot prove it. The absence of evidence becomes evidence of absence.
What actually builds a defensible compliance position is operational consistency over time. A legionella case study from our own work illustrates the point: a commercial premises with a well-documented control programme was able to provide complete temperature records for every monitored outlet going back two years within 24 hours of a suspected case being flagged. That documentation not only supported an accurate RIDDOR assessment but also demonstrated to investigators that the system was well-managed. The outcome was very different from sites where records were incomplete.
Regular staff training on the distinction between legionella control duties and reporting obligations is not a nice-to-have. It is the mechanism through which your compliance programme actually functions under pressure. People who understand why they are recording temperatures and what those records are for make far fewer omissions than people following a process they do not understand.
Supporting your legionella compliance and RIDDOR reporting needs
Managing legionella risk across healthcare and commercial properties while staying RIDDOR-ready requires more than good intentions. It requires a structured, documented, and consistently maintained programme that holds up under scrutiny when it matters most.

At Bespoke Compliance Solutions, we provide bespoke legionella risk assessments tailored to your sector, premises, and water systems, giving you a clear, current baseline for both control and reporting decisions. Our system disinfection and flushing services address contamination risks before they become incidents. For facilities where manual monitoring creates gaps, our automated water temperature monitoring solution delivers continuous, timestamped data that provides exactly the kind of evidence base a defensible RIDDOR report depends on. We work alongside your team to make compliance straightforward and your records inspection-ready at all times.
Frequently asked questions
Do all positive legionella test results require RIDDOR reporting?
No. RIDDOR reporting is triggered only by confirmed legionellosis disease in employees exposed to likely contaminated systems, not by positive test results alone. A positive water sample is a control issue requiring immediate remediation, not a reportable disease event.
Who reports legionellosis cases to public health authorities in the UK?
Registered medical practitioners report confirmed and probable legionellosis cases to the UKHSA within 3 days under Health Protection Notification rules, separate from the employer’s RIDDOR duty. You cannot rely on this clinical notification to fulfil your own RIDDOR obligation.
What water temperatures help prevent legionella growth?
To control legionella, hot water should be stored above 60°C and distributed above 50°C, while cold water should be kept below 20°C. These thresholds prevent the 20°C to 45°C temperature range in which legionella bacteria multiply most rapidly.
What records support RIDDOR reporting for legionellosis?
Maintaining timely logs of water temperatures, flushing schedules, and cleaning provides essential evidence that systems were controlled during the period relevant to any employee legionellosis case. As HSE monitoring guidance confirms, these records form the evidential backbone of any exposure assessment and RIDDOR reporting decision.
Recommended

Comments